An overview:
A new deadly narcotic that you should be aware of is on the streets as the American opioid problem worsens.
Xylazine, also referred to as “tranq,” is a non-opioid sedative, analgesic drug that is mostly combined (adulterated) and added to other opioid drug such as cocaine, heroin, and fentanyl. Blending tranq aids in developing, amplifying, or simulating the effects of these medications. In actuality, up to 15% of fentanyl tests now contain Tranq.
However, there are harmful, possibly fatal impacts on your health that could result from being exposed to this combination of substances. It’s been called a “zombie drug” since it can leave your skin with such horrible wounds (necrotic skin ulcers).
All the information you require about Tranq Philly and its consequences is here.
Xylazine, or Tranq: What Is It?
What is Tranq? Well, in 1962, everyone saw the introduction of Tranq by Bayer HealthCare Pharmaceuticals. Its intended function is as a depressant for the central nervous system. It is frequently used by veterinarians to sedate, calm, or relax muscles in animals such as horses, dogs, and cats. The FDA has not cleared its usage in men.
Typically, a transparent liquid is sold with it. The medications take effect in animals in minutes and have a maximum duration of four hours. Brand names such as Anased, Chanazine, Rompun, and Sedazine are employed to promote it.
Is Tranq Approved or legal?
Federally controlled substances do not include tranq dope. This indicates that using it independently is not prohibited under federal law. With a veterinarian’s prescription, you can obtain it.
However, the regulations around it are changing, and some states are making the restrictions more stringent. For instance, Xylazine was classified as a prohibited substance in 2017 by a bill approved in New York, making it unlawful to consume or sell the drug.
What Is the Use of Tranq?
Most street-finding Tranq is combined with cocaine, fentanyl, or heroin to change or intensify the effects of the drug. It produces a euphoric or “high” feeling akin to that of opiates.
“Speedball” is the name given to the narcotic when it is mostly combined with heroin and cocaine. In addition to Tranq or “zombie dope,” it goes by additional street names in the United States, such as “sleep cut” or “tranq dope.” It is known as “anesthesia de caballo,” or horse anesthesia, in Puerto Rico, where Xylazine has been implicated in the supply of opioids since the early 2000s.
The following are some ways that users of this tainted medicine enter their bloodstream:
- Snorting
- Smoking
- Injecting
- Eating
- Swallowing
- Breathing
There are also traces of Xylazine in other medications. Benzodiazepines, alcohol, methadone, gabapentin, and prescription painkillers might all fall within this category. Zombie drug Philadelphia misuse, accidental or deliberate poisoning, and attempted sexual assaults have all involved the usage of Xylazine.
What Impact Is Tranq Having on People?
Overdosing on medications that have traces of Tranq in them can have harmful negative effects. An overdose can be fatal in extreme circumstances.
Transq exposure can resemble an opioid overdose quite a bit. It may include:
- Cessation of central nervous system activity
- sedative
- Breathe slowly.
- Hypotension, or low blood pressure
- Bradycardia, or a slow heart rate
- severe, excruciating skin abscesses and ulcers (necrotic skin lacerations)
- delayed healing of wounds
- Skin infections that are recurring, chronic, or getting worse
- Eye conditions such as miosis or narrow pupils
- Low glucose levels, or hypoglycemia
- elevated glucose levels (hyperglycemia)
- Tiredness Amnesia
Injecting Tranq typically results in severe skin ulceration. Nevertheless, the gashes may appear on different areas of your body depending on where you use Tranq to puncture your skin.
If you have any of these symptoms, get medical help immediately by calling 911 or going to the closest hospital.
How Much Time Do Human Tranq Effects Last?
According to accounts, the effects of a tranq overdose in humans can persist anywhere from eight to seventy-two hours (3 days).
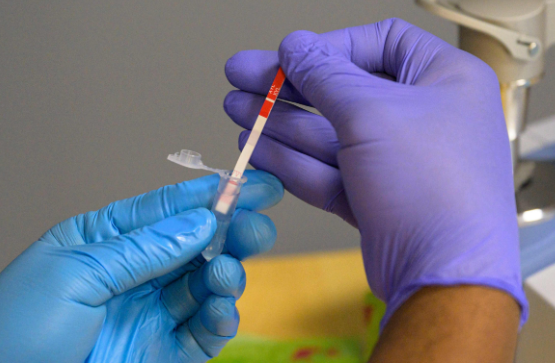
Does Tranq Appear in Drug Test Results?
There are no quick or easy drug tests to look for tranq residue.
As of right now, toxicological screens and standard drug tests that look for opioids or other illicit substances don’t reveal Tranq Philadelphia. To find any xylazine residue in your system, your doctor will need to perform additional investigations or blood work.
Your doctor will do a skin biopsy if you have significant skin lesions. To determine the cause, they will take a sample of the peeling skin tissue from you and examine it under a microscope.
The following tests can identify Tranq:
- chromatography using thin layers
- Mass spectrometry and gas chromatography
How Are Overdoses of Tranq Treated?
Transq exposure and overdose lack a straightforward counteragent, in contrast to common opioids like fentanyl or heroin.
However, because Tranq is frequently combined with opioids, first responders will inject naloxone, sometimes known as Narcan, to counteract the effects of the opioid. Naloxone, however, is not a good treatment for tranq exposure.
Indeed, the potency of Tranq can be so great that it will take multiple doses of naloxone to counteract the effects of the opioids in the cocktail and bring an exposed person back to consciousness. Yet, it doesn’t address the problems with breathing or the heart that Tranq brings on. Furthermore, there is no medication to help with withdrawal symptoms.
Safety Advice for Using Tranq
If you use illegal horse tranquilizer drugs like opioids regularly, you may unintentionally or purposely come into contact with or ingest Tranq. Use them carefully because they might have harmful impacts on your health. The best course of action is to educate yourself on opioids, illegal drugs, and how to handle potentially dangerous side effects if you should experience any of these.
An Ending:
The emergence of Xylazine, or “tranq,” amid the intensifying opioid crisis in the United States presents a greater risk of illicit drug usage. It was once used as a sedative for animals, but it’s now mixed into other illicit substances to increase danger. Due to its “zombie drug” status and potential to cause severe skin wounds, awareness is becoming increasingly crucial. As laws change, users must exercise extreme caution and education to protect their health from this deadly mix. Symptoms require immediate medical attention, underscoring the significance of education in creating an atmosphere of security.
Also Read: The Dangers of At-Home Drug Detox and the Need for Professional Care